Liver iron overload symptoms may include fatigue, abdominal pain, joint discomfort, weakness, and abnormal liver function. Recognizing early signs of excess iron buildup is important for preventing liver damage, managing iron levels, and protecting long-term overall health.
Introduction to Liver Iron Overload
Understanding how excess iron impacts your body starts with looking at the underlying causes. For many people, iron accumulation happens slowly over decades, often driven by genetics or required medical treatments for other conditions.
What is hemochromatosis?
Hemochromatosis is the most common cause of iron overload. It is a genetic disorder that disrupts how your body handles iron absorption. Normally, your intestines only absorb the exact amount of iron your body needs from the food you eat. If you have hemochromatosis, your body misses the signal to stop. It absorbs multiple times the normal amount of iron every day.
Because the human body lacks a natural way to flush out large amounts of extra iron, the mineral builds up. Primary hemochromatosis is inherited, meaning it passes down through families. Secondary hemochromatosis, on the other hand, happens due to external factors. For example, people with different types of thalassemia often develop iron overload because they require frequent blood transfusions.
Importance of early detection for liver iron overload symptoms
Finding out you have too much iron early on can literally save your life. The initial liver iron overload symptoms are notoriously vague. They often mimic everyday complaints like feeling tired or having sore joints. Because of this, patients frequently go undiagnosed until the iron has already caused significant harm.
When you catch iron overload before it triggers severe liver scarring, the condition is highly manageable. Simple treatments can reduce the iron stores back to normal levels. This proactive approach prevents the development of irreversible conditions and keeps your vital organs functioning correctly.
Understanding Iron Metabolism
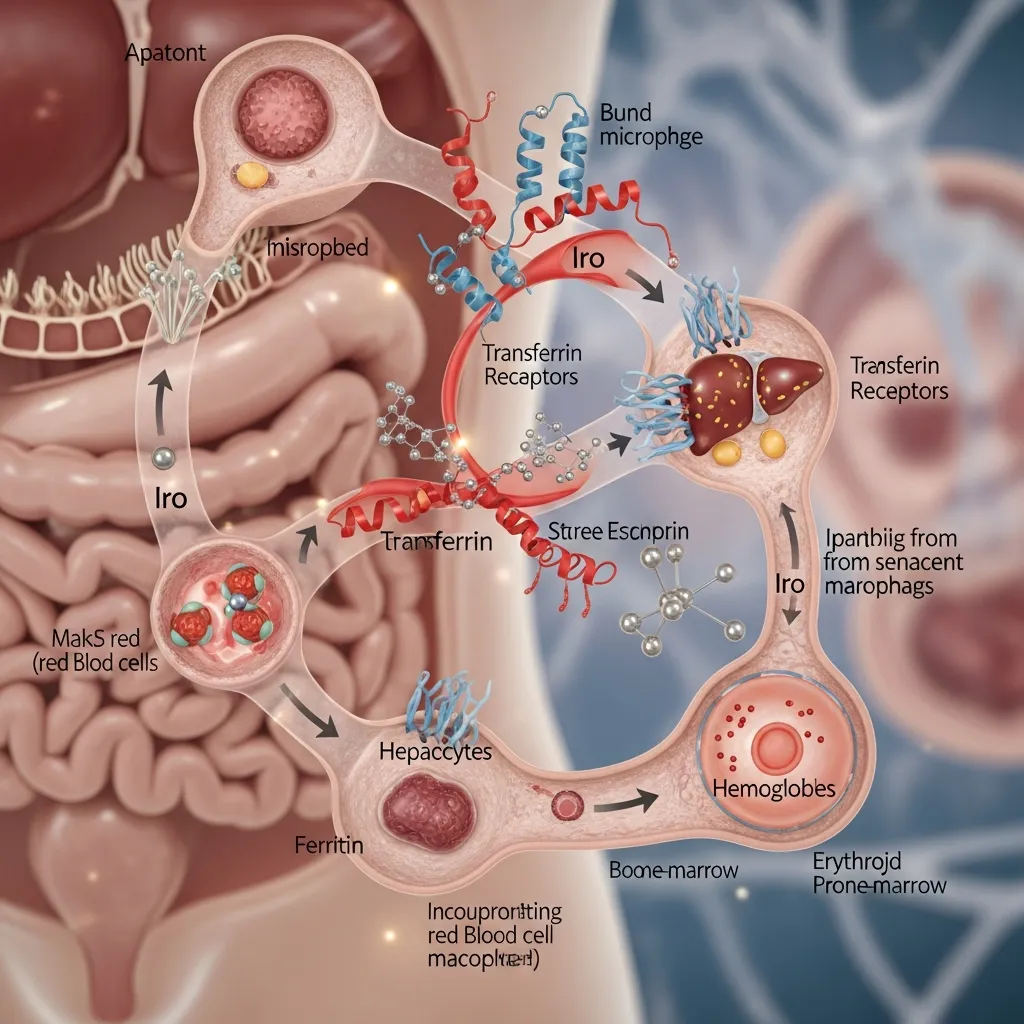 To understand why liver iron overload symptoms develop, it helps to know how the body normally manages iron. Iron is an essential mineral needed for oxygen transport, energy production, and healthy cell function. However, too much iron can become toxic, especially when it builds up in organs such as the liver.
To understand why liver iron overload symptoms develop, it helps to know how the body normally manages iron. Iron is an essential mineral needed for oxygen transport, energy production, and healthy cell function. However, too much iron can become toxic, especially when it builds up in organs such as the liver.
The body uses a tightly controlled system to keep iron levels balanced. When this system fails, excess iron accumulates and may lead to liver iron overload symptoms such as fatigue, abdominal pain, weakness, and liver damage.
How the Body Regulates Iron
When you eat iron-rich foods such as red meat, beans, spinach, or fortified cereals, iron is absorbed mainly through the small intestine. The body only absorbs the amount it needs under normal conditions.
A hormone called hepcidin, produced by the liver, acts as the main regulator of iron balance. When iron stores are sufficient, hepcidin levels rise and reduce iron absorption. When iron levels are low, hepcidin decreases so the body can absorb more iron.
Once absorbed, iron attaches to a transport protein called transferrin. This protein carries iron through the bloodstream to areas where it is needed, especially the bone marrow for red blood cell production.
Unused iron is stored inside a protective protein called ferritin. The liver is the body’s main iron storage organ, which is why it is most affected when excess iron builds up. When storage becomes excessive, liver iron overload symptoms may begin to appear.
What Happens in Iron Overload
In iron overload disorders, the normal balance of iron metabolism is disrupted. The body continues absorbing iron even when it already has enough stored.
This commonly happens in hereditary hemochromatosis, where genetic changes reduce hepcidin function. As a result, the intestines keep absorbing iron continuously, causing iron levels to rise over time.
Repeated blood transfusions can also cause iron overload because each transfusion adds more iron to the body. This is common in conditions such as thalassemia or chronic anemia.
As ferritin storage capacity becomes full, extra iron begins depositing directly into tissues and organs. The liver receives the greatest burden because it stores most of the body’s iron.
Why Excess Iron Damages the Liver
Free iron molecules are highly reactive and can damage healthy liver cells through oxidative stress. This process injures cell membranes, proteins, and DNA, leading to inflammation and scarring.
Over time, untreated excess iron may cause:
- Fatty liver changes
- Chronic inflammation
- Liver fibrosis
- Cirrhosis
- Increased risk of liver cancer
These complications often begin after early liver iron overload symptoms are ignored or left untreated.
Common Liver Iron Overload Symptoms
As iron continues to build up, many people begin to notice symptoms gradually. Common liver iron overload symptoms include:
- Ongoing fatigue
- Weakness
- Pain in the upper right abdomen
- Joint pain
- Unexplained weight loss
- Elevated liver enzymes
- Skin darkening
- Reduced appetite
Some people may have no symptoms in the early stages, making routine testing important.
Importance of Early Detection
Recognizing liver iron overload symptoms early can help prevent severe liver damage. Blood tests such as ferritin, transferrin saturation, and liver function tests are commonly used to detect excess iron. MRI scans may also measure iron levels in the liver.
With early treatment, iron levels can often be reduced before permanent complications occur.
Diagnosing Liver Iron Overload
If you or your doctor suspect iron accumulation, a quick diagnosis is essential. Medical professionals use several reliable methods to check your iron levels and evaluate organ health.
Blood tests (ferritin, transferrin saturation)
The diagnostic process almost always begins with simple blood work. If you are preparing for a checkup, understanding the standard thalassemia test guide can give you an idea of how doctors look at blood panels.
Doctors look at two specific measurements. The first is transferrin saturation, which shows how much iron is currently bound to the transport proteins in your blood. A high saturation percentage indicates your body is absorbing too much iron. The second measurement is serum ferritin. High ferritin levels show that your body has a massive stockpile of stored iron.
Genetic testing
If your blood tests show high iron levels, the next step is usually a DNA test. A simple blood draw or cheek swab can reveal if you carry the specific gene mutations responsible for hemochromatosis. The most common mutations happen on the HFE gene. Identifying this genetic link confirms the diagnosis and helps determine if your family members should also get tested.
Liver biopsy and imaging
To see exactly how much iron is in the liver and check for tissue damage, doctors use specialized imaging or biopsies. Advanced MRI scans can accurately measure the concentration of iron inside the liver without any needles. In some cases, a doctor may perform a liver biopsy. They remove a tiny piece of liver tissue using a thin needle and examine it under a microscope. This confirms the exact degree of scarring or cirrhosis present.
Complications of Untreated Iron Overload
Ignoring liver iron overload symptoms allows the toxic metal to silently destroy your body’s most important systems. Without medical intervention, the long-term consequences are severe and often life-threatening.
Liver damage (cirrhosis, cancer)
The liver bears the brunt of untreated iron toxicity. Chronic inflammation eventually replaces healthy, functional liver cells with rigid scar tissue. This advanced scarring is called cirrhosis. A cirrhotic liver cannot filter toxins, process medications, or aid in digestion effectively. A complete guide to organ damage shows that patients with cirrhosis also face a dramatically increased risk of developing hepatocellular carcinoma, a deadly form of liver cancer.
Heart problems
When the liver runs out of room, iron spills into the heart muscle. This disrupts the heart’s electrical signals and weakens its pumping ability. Patients may develop arrhythmias, causing their heart to beat too fast or irregularly. Over time, the toxic environment leads to cardiomyopathy and congestive heart failure. Managing these heart problems requires immediate medical attention to prevent fatal cardiac events.
Diabetes
The pancreas, a small organ behind the stomach, is highly sensitive to iron. Iron deposits destroy the beta cells responsible for making insulin. When the body cannot produce insulin, blood sugar levels skyrocket, resulting in diabetes mellitus. This complication is so common in advanced hemochromatosis that the condition is sometimes referred to as “bronze diabetes” due to the accompanying skin color changes.
Joint and endocrine issues
Iron buildup severely disrupts the endocrine system, the network of glands that produce hormones. This can lead to hypothyroidism, causing extreme fatigue and weight gain. Damage to the pituitary gland often results in severe sexual dysfunction and reproductive issues. These adult complications require specialized hormone therapies to manage properly. Additionally, the joint damage caused by iron deposits often leads to permanent arthritis, necessitating pain management and sometimes joint replacement surgeries.
Treatment Options
The good news is that iron overload is highly treatable. Once a doctor confirms the diagnosis, they will create a plan to safely remove the excess iron and protect your organs from further harm.
Phlebotomy
Therapeutic phlebotomy is the most common and effective treatment for genetic hemochromatosis. It works exactly like donating blood. A medical professional removes about a pint of blood from your arm on a regular schedule.
Because red blood cells contain a massive amount of iron, removing blood forces your body to tap into your liver’s iron stores to make new red blood cells. In the beginning, you might need a phlebotomy once or twice a week. Once your iron levels drop to a safe range, you will only need maintenance treatments a few times a year.
Chelation therapy
For people who cannot undergo phlebotomy—such as those with severe anemia or thalassemia—doctors use iron chelation therapy. Chelators are prescription medications taken orally or through an infusion. These drugs circulate in the bloodstream, bind to free iron molecules, and allow your body to excrete the iron safely through your urine or stool. You can learn more about how this specific treatment protects organs by visiting the Cleveland Clinic’s resources on chelation.
Dietary considerations
While diet alone cannot cure iron overload, making smart food choices helps slow down the accumulation process. Doctors generally advise patients to avoid taking any vitamin pills containing iron or vitamin C. Vitamin C significantly increases how much iron your intestines absorb from food.
You should also limit your intake of iron-fortified cereals and raw shellfish. Raw shellfish carries a specific bacteria that can cause fatal infections in people with high iron levels and liver damage.
Living with Hemochromatosis
Being diagnosed with an iron overload disorder means you will need to pay close attention to your health for the rest of your life. However, with a few adjustments, you can maintain a completely normal and active lifestyle.
Lifestyle adjustments
Protecting your liver is your highest priority. Since your liver is already under stress from iron, you should strictly limit or completely eliminate alcohol. Alcohol accelerates liver scarring and drastically increases the risk of cirrhosis.
Staying physically active and maintaining a healthy weight also supports overall liver function and helps manage blood sugar levels, reducing the risk of diabetes. According to the National Institutes of Health (NIH), a balanced lifestyle goes a long way in supporting individuals managing chronic genetic disorders.
Regular monitoring
Consistency is key when dealing with iron overload. You will need to build a strong relationship with your healthcare team. Make sure you attend all scheduled blood tests to monitor your ferritin and transferrin saturation levels. These routine checks ensure your maintenance treatments are working correctly.
You should also undergo regular liver ultrasounds or MRI scans to keep a close eye on any structural changes. If you develop any new symptoms, report them to your doctor immediately so they can adjust your treatment plan.
Proactive Management of Liver Iron Overload
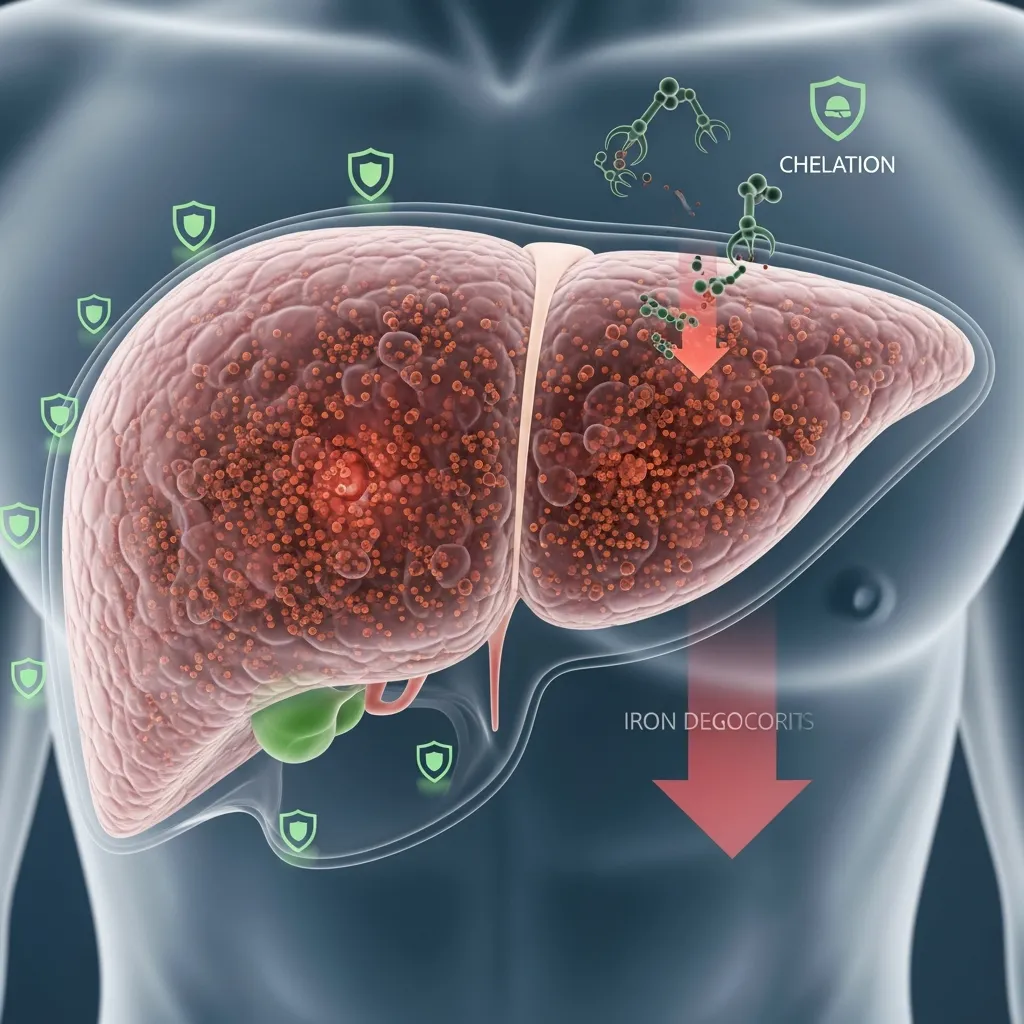 Taking control of your health requires vigilance and education. Understanding how iron moves through your body gives you the power to spot warning signs early.
Taking control of your health requires vigilance and education. Understanding how iron moves through your body gives you the power to spot warning signs early.
Recap of key takeaways
Liver iron overload happens when the body absorbs too much iron and stores the toxic excess in vital organs. Conditions like hemochromatosis and frequent blood transfusions are the primary culprits. The symptoms start out mild—fatigue, joint pain, and abdominal discomfort—but can rapidly progress to severe liver disease, heart failure, and diabetes.
Diagnosis is straightforward, usually requiring basic blood work and a genetic test. Treatments like therapeutic phlebotomy and chelation therapy are highly successful at clearing out the excess iron and halting organ damage.
Encouragement for early consultation and management
You do not have to wait for severe symptoms to disrupt your life. If you have a family history of hemochromatosis or experience unexplained, persistent fatigue and joint pain, speak to your doctor.
Ask for a simple iron panel blood test. Catching liver iron overload symptoms in their earliest stages ensures that you can clear the excess iron before any permanent damage occurs. With regular monitoring and a proactive treatment plan, you can protect your liver and look forward to a healthy, vibrant future.


 Iron overload often affects more than just the liver. Once storage systems become overloaded, iron deposits in other organs and tissues, creating widespread health issues.
Iron overload often affects more than just the liver. Once storage systems become overloaded, iron deposits in other organs and tissues, creating widespread health issues.